The landscape of healthcare has irrevocably shifted. Telehealth, once a niche practice, has surged into the mainstream, transforming how patients access care and providers deliver it. According to a McKinsey & Company report, telehealth utilization grew 78 times during the first three months of the COVID-19 pandemic alone. While the danger of a pandemic is now gone, both healthcare professionals and patients are much more open to embracing telehealth and telemedicine in their lives and work.
This rapid change, however, necessitates a crucial focus: the utmost protection of patient privacy and data security as a cornerstone of custom healthcare software development.
At the heart of this responsibility lies HIPAA, the Health Insurance Portability and Accountability Act. Enacted to safeguard sensitive patient information, HIPAA applies equally to both in-person and virtual healthcare encounters. Embracing its guidelines in the telehealth realm is not just a legal obligation; it’s a cornerstone of building trust and confidence in this evolving landscape.
In this article, we’ll try to look into the intricacies of HIPAA compliance for telehealth, dissect the key regulations, explore practical implementation strategies, and address common concerns about data security in the virtual healthcare space.
HIPAA Compliance for Telehealth
While the benefits of telehealth are undeniable, navigating the legal landscape surrounding patient data security can feel like navigating a maze. Fear not, for understanding HIPAA in the context of virtual healthcare isn’t a herculean task. This section equips you with the essential knowledge to confidently ensure a compliant and secure telehealth experience.
Protected Health Information (PHI)
At the core of HIPAA lies the concept of Protected Health Information (PHI). This encompasses any individually identifiable information related to a patient’s health status, medical history, and treatment plans. Whether exchanged through video consultations, text messages, or electronic medical records, all PHI transmitted in a telehealth setting falls under HIPAA’s protective umbrella.
Key HIPAA Rules
Understanding the relevant HIPAA rules empowers both healthcare providers and software developers to design and utilize secure telehealth solutions. Here are the key regulations to keep in mind:
- Security: This rule sets forth robust technical, physical, and administrative safeguards to protect ePHI (electronic PHI) from unauthorized access, disclosure, or misuse. Think of it as building a secure digital fortress around your patients’ data.
- Privacy: This rule governs how PHI can be used and shared, requiring patient authorization for most disclosures. Custom healthcare software providers can build functionality that facilitates clear consent management, ensuring patients stay informed and empowered.
- Breach Notification: In the unfortunate event of a data breach, this rule mandates prompt notification to affected individuals and regulatory authorities. Proactive cybersecurity measures and data breach response plans are crucial to mitigate risks and maintain patient trust.
Building Trust and Confidence
HIPAA compliance isn’t just a checkbox exercise; it’s a cornerstone of building trust and confidence in telehealth. Healthcare software developers have a vital role to play in creating user-friendly and secure platforms that empower both providers and patients to navigate HIPAA regulations seamlessly.
By embracing transparency, incorporating robust security features, and providing clear communication on data handling practices, software providers can position themselves as reliable partners in the quest for secure and accessible telehealth.
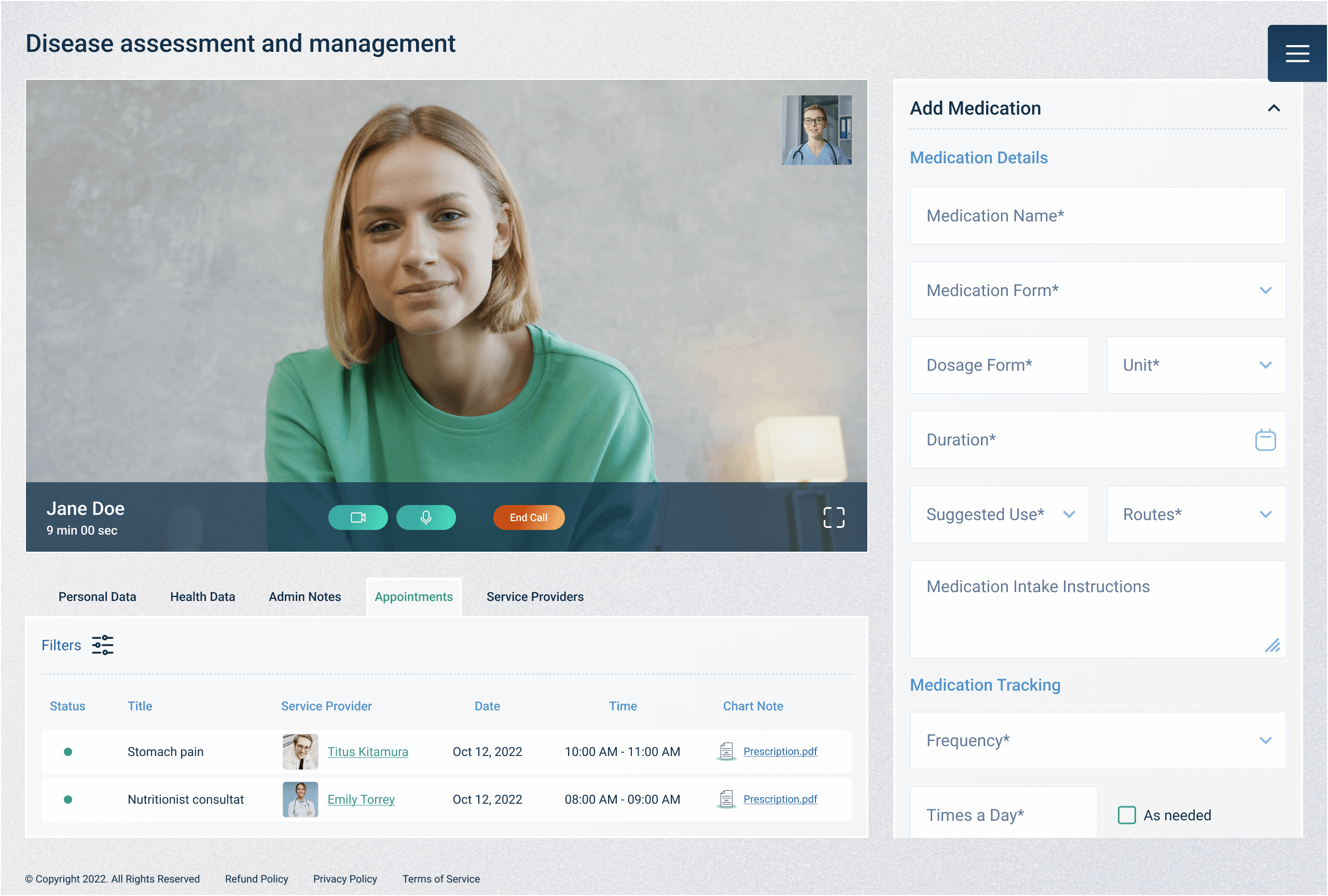
Implementing Secure Telehealth Solutions
Now, let’s delve into the practical steps of implementing secure solutions. Choosing the right technology and implementing robust security measures are essential to ensure patient data remains safe and private throughout the virtual healthcare journey.
Selecting HIPAA-Compliant Technology
The foundation of secure telehealth lies in choosing technology that adheres to HIPAA compliance standards. This goes beyond simply ticking a box; it requires rigorous vetting of software providers and careful evaluation of the security features they can offer. Look for providers who:
- Demonstrate a clear commitment to HIPAA compliance: Proven expertise in building healthcare software, especially for HIPAA, should be a priority.
- Offer robust data encryption: Both data in transit (during video calls) and data at rest (stored data) should be encrypted using industry-standard algorithms.
- Provide granular access controls: Focus on the software where only authorized personnel have access to PHI by implementing user roles and permissions.
- Regularly update software and security protocols: Staying ahead of evolving cyber threats requires continuous updates to software and security measures.
By adhering to these recommended practices, healthcare providers and software developers can work together to create a secure and trustworthy environment for telehealth. Remember, HIPAA compliance is an ongoing process, not a one-time achievement. Continuous vigilance and a proactive approach are key to safeguarding patient data in the ever-evolving digital landscape.
Addressing Patient Concerns and Building Trust
While telehealth offers undeniable benefits, patient concerns about data security and privacy can present a formidable barrier to adoption. Addressing these concerns head-on and building trust is crucial for fostering a thriving telehealth ecosystem.
Understanding Patient Anxieties
Patients entrust healthcare providers with their most sensitive information. In the virtual setting, anxieties about data breaches, unauthorized access, and potential misuses of their data are understandable. Common concerns include:
- Security of video conferencing platforms: Fear of hacking or unauthorized recordings of consultations.
- Data storage and protection: Worry about where data is stored and how it’s protected.
- Transparency and control: Lack of clarity about how their data is used and shared.
Building Trust Through Transparency and Communication
Transparency and open communication are the cornerstones of building trust in telehealth. Here are some key strategies:
- Clearly explain HIPAA compliance: Educate patients about HIPAA regulations and how their data is protected.
- Provide detailed information about your security measures: Outline the steps you take to safeguard patient data, including encryption, access controls, and data breach response plans.
- Obtain informed consent: Clearly explain how their data will be used and obtain explicit consent for any sharing beyond routine care.
- Offer easy-to-access resources: Provide readily available materials explaining your privacy policies and data handling practices.
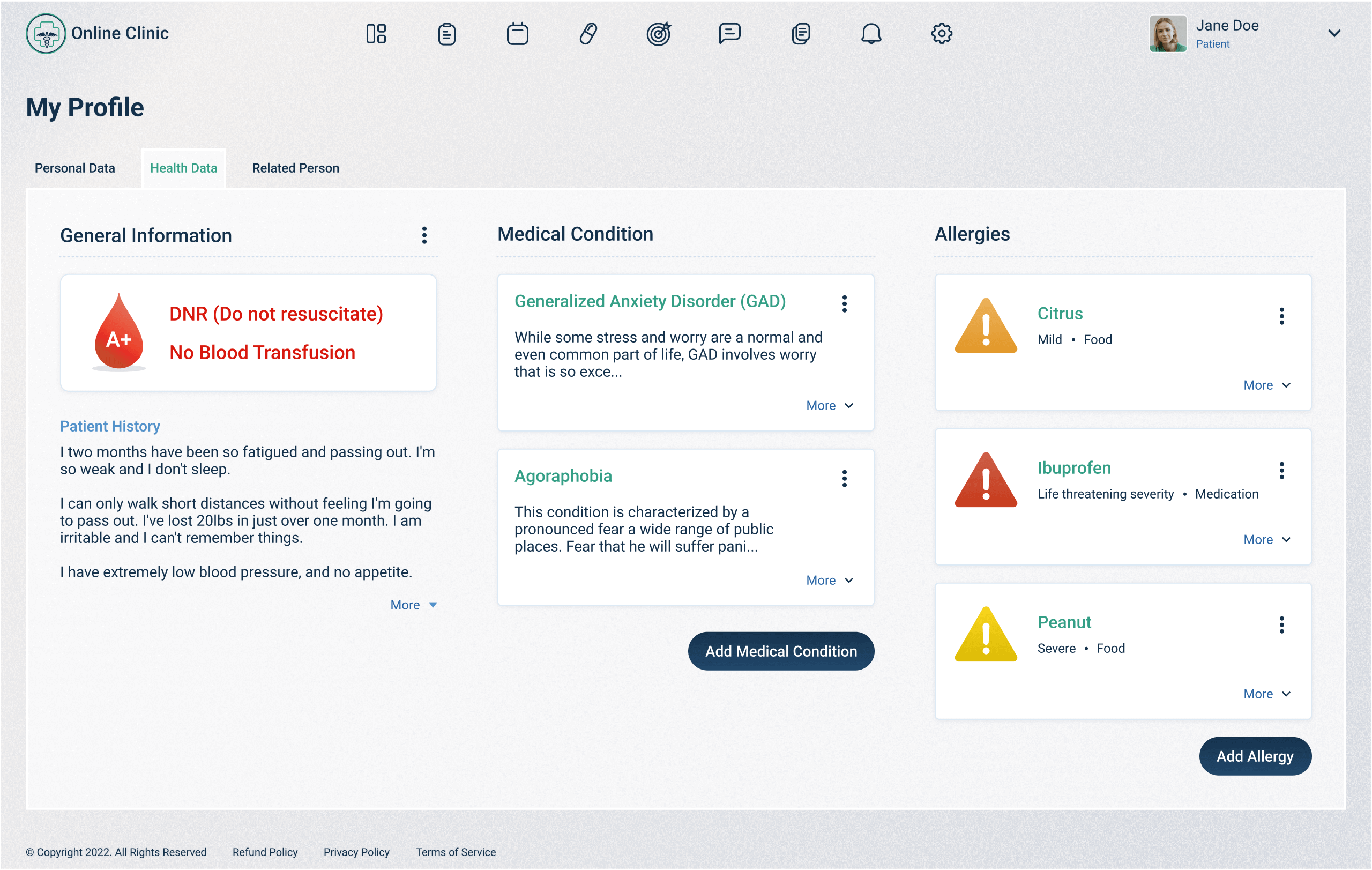
Building Trust Through User-Friendly Design
Sufficient investment of time and resources into the product design stage for your telehealth platform also plays a crucial role in building trust. Consider these elements:
- Simple and intuitive user interface: Make it easy for patients to navigate the platform and manage their data.
- Clear data access and control features: Provide patients with clear mechanisms to exercise their HIPAA rights to access and amend their data.
- Prominent security indicators: Display visual cues, such as encryption and privacy badges, to reassure patients of their data’s safety.
By embracing these strategies, healthcare providers and software developers can foster a trusting environment where patients feel comfortable and empowered to engage in telehealth. As an ongoing process, building trust requires continuous evaluation and improvement of your approach to secure data handling and open communication.
The Future of Secure Telehealth
As technology advances and patient expectations shift, the future of secure telehealth promises exciting possibilities while also presenting new challenges to overcome.
Innovation and Technology
- Artificial intelligence (AI): AI-powered tools can enhance diagnostic accuracy, personalize treatment plans, and streamline administrative tasks, all while adhering to stringent privacy regulations.
- Blockchain technology: Securely storing and sharing medical records on a decentralized blockchain could offer enhanced transparency and control over patient data.
- Internet of Medical Things (IoMT): Wearable devices and remote monitoring tools can provide real-time patient data, but robust security measures are crucial to prevent unauthorized access and data breaches.
Building a Future of Trust and Accessibility
Ultimately, the future of secure telehealth hinges on building trust and ensuring equitable access for all. This requires:
- Maintaining transparency and open communication with patients: Educate them about how their data is protected and involve them in decision-making processes.
- Addressing the digital divide: Bridging the gap in access to technology and ensuring inclusivity for all populations.
- Promoting international collaboration and data standardization: Facilitating secure telemedicine across borders for improved global healthcare outcomes.
By embracing innovation responsibly, prioritizing data security, and fostering trust, we can ensure that the future of telehealth is bright, accessible, and secure for all.
Additional Information
With a topic as complex as developing custom software for healthcare, and telehealth in particular, it is hard to cover all angles. Let’s take a look at some of the questions that we, as a healthcare software provider, have faced in the past:
1. Q: I’m building a healthcare software platform. Do I need to worry about HIPAA compliance?
A: Yes, if your platform handles any Protected Health Information (PHI) of patients located in the US, then HIPAA compliance is essential. This includes information like medical records, diagnoses, and treatment plans. Even basic contact information can fall under PHI if linked to medical history.
2. Q: What are the key steps to ensuring my software is HIPAA-compliant?
A: The journey to HIPAA compliance involves several steps:
- Conduct a security risk assessment: Identify and mitigate potential vulnerabilities in your platform.
- Implement robust security measures: This includes data encryption, secure access controls, and audit trails.
- Choose reliable third-party vendors: Ensure any partners handling PHI also adhere to HIPAA regulations.
- Develop clear privacy policies and procedures: Inform users about data practices and obtain informed consent.
- Train your staff and developers: Educate everyone involved about HIPAA requirements and data security best practices.
3. Q: I want to expand my software to Canada/EU. Do I need to worry about HIPAA?
No, HIPAA only applies to healthcare data of individuals in the US. However, Canada and the EU have their own data privacy regulations, like PIPEDA and GDPR, respectively, not to mention a plethora of other regional regulations, that can include specific requirements for each country within the EU.
These regulations have different requirements than HIPAA, so you’ll need to ensure your software complies with the specific regulations of your target markets. Partnering with healthcare software development companies with relevant exertise can help navigate these intricacies.
The Takeaway
The rise of telehealth has transformed healthcare, offering accessibility, convenience, and improved patient outcomes. Yet, this transformation hinges on a fundamental cornerstone: the utmost protection of patient privacy and data security. By embracing HIPAA compliance as a guiding principle and adopting robust security measures, we can pave the way for a future where telehealth in the US thrives with confidence and trust.
This journey requires a collective effort. Healthcare providers, software developers, policymakers, and patients all have a role to play. By building secure and user-friendly platforms, adhering to ethical data practices, and promoting ongoing communication about privacy rights, we can build a future where telehealth empowers healthier lives for all.
Embrace the possibilities, champion security, and let’s build a thriving and secure telehealth ecosystem together. Contact us and share the details with your project so we can embark on this journey together!